 More than a third of adults in the United States have obesity, and people who live in socioeconomically disadvantaged neighborhoods with lower-income and less-educated populations have a higher risk of obesity. This includes older adult populations, which continue to grow and increase the demand for health care. In fact, Americans born between 1946 and 1962 have the highest obesity rate of any age group, and as they age, their high obesity rates could make their health care more challenging. An NIMHD-supported study has shown that using a neighborhood-based index of socioeconomic disadvantage measures could help predict obesity risk in older adults.
More than a third of adults in the United States have obesity, and people who live in socioeconomically disadvantaged neighborhoods with lower-income and less-educated populations have a higher risk of obesity. This includes older adult populations, which continue to grow and increase the demand for health care. In fact, Americans born between 1946 and 1962 have the highest obesity rate of any age group, and as they age, their high obesity rates could make their health care more challenging. An NIMHD-supported study has shown that using a neighborhood-based index of socioeconomic disadvantage measures could help predict obesity risk in older adults.
The study included more than 4,000 Medicare beneficiaries age 65 or older who received care from the University of Missouri Health System between 2013 to 2014. The researchers used the Area Deprivation Index (ADI), a tool to measure neighborhood disadvantage based on 17 markers of socioeconomic status, such as income and poverty levels, education level, and employment. Each participant had an ADI score assigned according to his/her mailing address. (See Figure 1, a U.S. map illustrating neighborhood disadvantage levels from ADI scores across the country.) Obesity was defined as body mass index of 30 or higher.
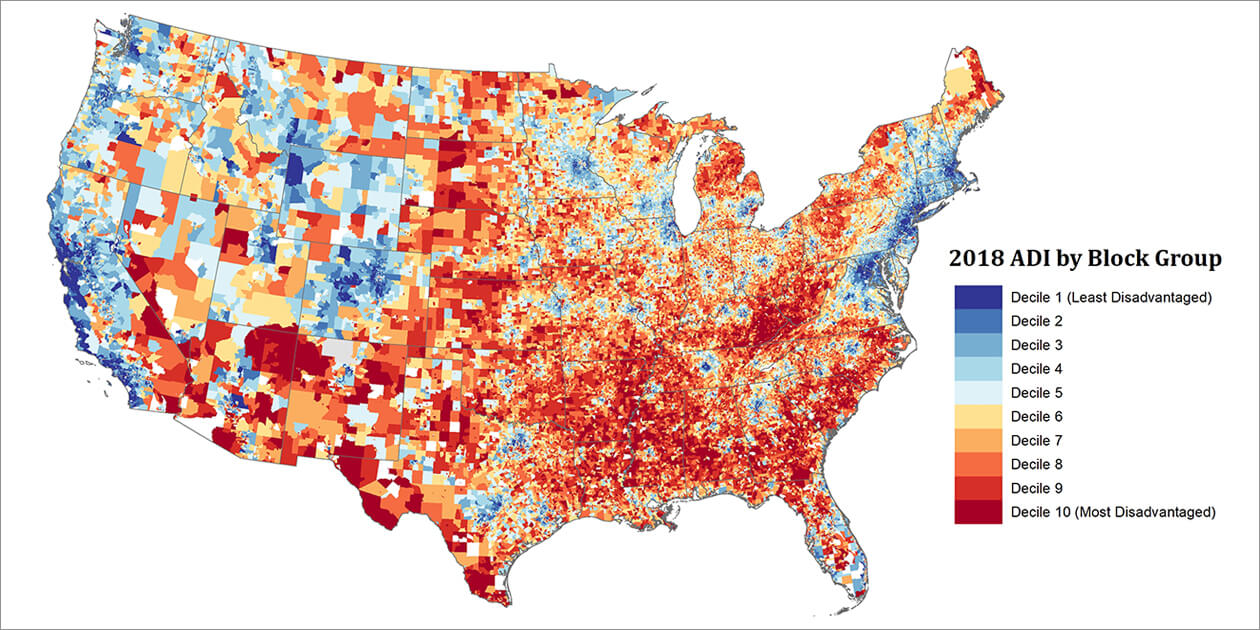
Image provided by the Health Services and Care Research Program, Department of Medicine, University of Wisconsin School of Medicine and Public Health.
Using the ADI, the researchers found that obesity was least common in the neighborhoods of least disadvantage. More disadvantaged neighborhoods were linked to higher rates of obesity. Medicare patients whose health records included no BMI data were more likely to live in the most disadvantaged areas.
Findings from this study support the use of the ADI to predict neighborhood socioeconomic disparities and obesity risk in older populations. Potential reasons for the higher obesity risk in neighborhoods of socioeconomic disadvantage include having fewer healthy food options and a lack of safe places to exercise. Policymakers could use this information to better distribute resources to communities that may benefit from increased access to fresh food, parks, and recreational areas. Health professionals can make sure that patients get their weight and BMI measured regularly. Professionals may also suggest ways for patients to eat healthier and exercise safely in their neighborhoods—especially for more vulnerable older adults.
Page updated January 14, 2022

